By Santa J. Bartholomew M.D. FAAP, FCCM
See Corresponding Case Study: Early Onset GBS Group B Strep
Group B Strep (GBS) is an organism that lives in the bowels and genitals of adults. In women group B strep lives in the vagina and does not cause illness in these women but as the infant comes through the birth canal, they can become infected causing great harm to the infant. Because of the catastrophic consequences to the infant, pregnant women are routinely checked for GBS and treated before the infant is born. Group B strep infections in infants come in two categories: early onset and late onset. It is only early onset that is transmitted via birth. There are many serotypes of this bacteria but only 6 cause significant disease.
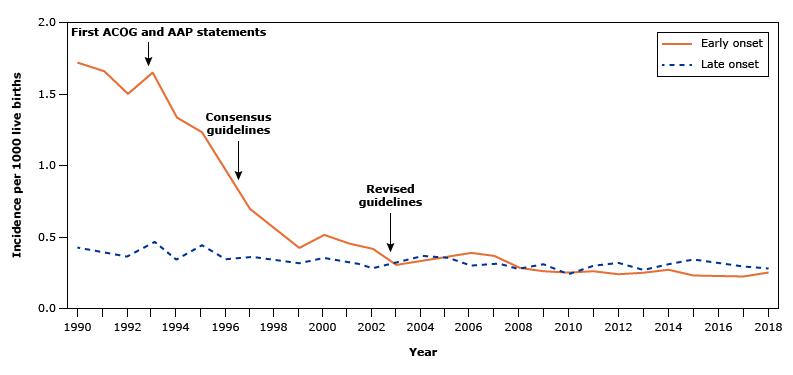
Neonatal or early onset GBS is acquired in utero via “silent” intraamniotic infection or via early rupture of membranes as well as passage through the vagina. When mothers are tested the higher quantities of bacteria in the vagina the greater risk of transmission to the infant. GBS infections are 0.5 per 1000 births with higher rates in black infants.
Despite many prevention policies enacted early onset GBS has not been eradicated in the USA. Late onset GBS disease has seen no decrease since the 1990’s and this is NOT prevented by treating the mother before birth.
Because of the catastrophic consequences to the infant, pregnant women are routinely checked for GBS and treated before the infant is born.
Risk Factors for Babies Getting GBS
- Colonized mother: transmission to the baby is 1 in 2 (50%)
- Prior delivery of a baby with GBS disease
- Delivery of a baby < 37 weeks gestation
- Rupture of membranes more than 18 hours
- Preterm labor with rupture of membranes
- Chorioamnionitis
- Fever in mom during labor
These risk factors have been incorporated into a prevention guideline to minimize risk to the newborn. This can be found at CDC website: ”Prevention of perinatal group B streptococcal disease.” These are imperative to follow as they dramatically decrease the risk of infection in the neonate.
Diagnosis of early-onset GBS disease in infants presents in fist week of life. It is crucial to review pregnancy and labor and delivery history as this can avoid catastrophic disease in the newborn.
- GBS can manifest as Generalized Sepsis: temperature instability, poor perfusion, lethargy, respiratory symptoms like grunting and fast breathing, shock.
- These babies can also have Persistent Pulmonary Hypertension in which blood does not flow easily to the lungs and can be quickly fatal disease.
- Pneumonia accounts for 10% of GBS disease in newborns and usually include CXR findings of alveolar disease, as well as low oxygen levels and signs of distress like fast breathing, gruntiong noises, periods of apnea.
- Meningitis Occurs in 5-10% of infants and presents as irritability, lethargy, poor feeding, vomiting, may or may not have respiratory symptoms.
When a baby is identified at high risk, there are two acceptable approaches to care listed below.
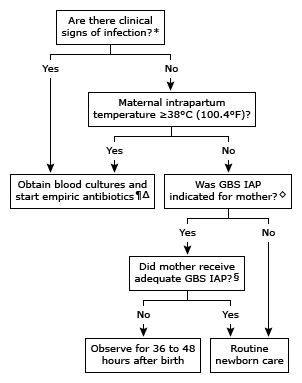
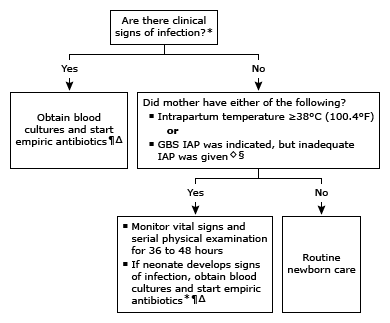
Treatment
In any infant who shows symptoms, an evaluation should be initiated immediately and should include:
- Blood cultures
- CBC with differential
- Lumbar puncture if there is clinical suspicion for sepsis
- CXR
- Urine culture
Treatment should be started with intravenous Ampicillin and Gentamicin.
Prognosis
Approximately 3% of infants infected with GBS die. Among the infants that survive the risk of dying remains elevated in the first decade of life as much as 3 times higher than uninfected infants. There is even higher mortality in infants that are preterm, weigh less than 2500 grams, present in shock, have apnea, seizures or low white count or platelets at presentation.
Even in the survivors they are at serious risk for cerebral palsy, seizures, neurologic disabilities, and blindness. Infants who have meningitis have the highest risk of disability, as high as 22-25%.
The key to good outcome is prenatal testing of mothers and treatment of mothers before birth. If this is not possible then high index of suspicion and observation +/- treatment in the neonate is paramount for good neonatal outcome.
