By Santa J. Bartholomew M.D. FAAP, FCCM
See Corresponding Case Study: Hemolytic Uremic Syndrome
Hemolytic Uremic Syndrome (HUS) is clinically defined as a triad including hemolytic anemia, thrombocytopenia, and acute kidney injury. This condition causes abnormal vessel wall and microvascular thrombosis (clotting) of the red blood cells. This causes destruction of blood platelets, thereby causing a low red blood cell count and ultimately acute kidney failure. This is a complex renal condition-affecting children typically under the age of 5. Some children recover from the disorder, however it is oftentimes fatal and if the child survives, 50% of the cases require short-term kidney replacement therapy.
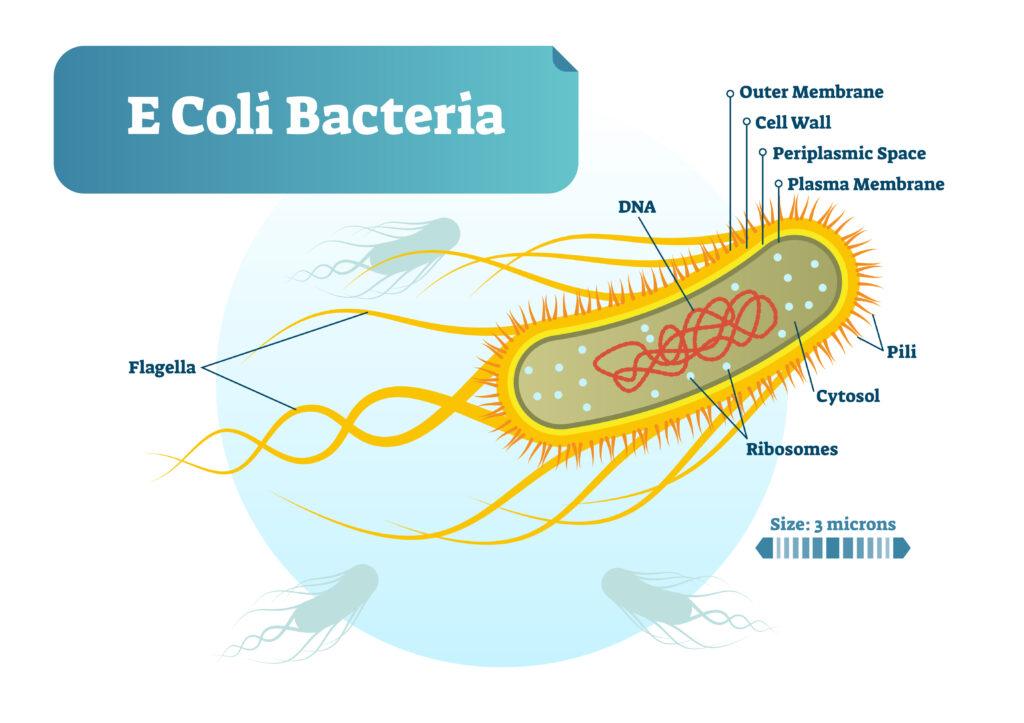
The causes of HUS is typically E. coli bacterial infection crossing into the intestines and thereby entering the bloodstream.
Classifications
HUS was previously defined as typical, primarily including the E. coli infection Shigella Toxin. Atypical HUS was caused by other factors. Ongoing medical research has given us a better and understanding of pathophysiological pathways. The condition is now classified as hereditary and acquired HUS. The focus of this paper will be on acquired HUS as this is more common. Hereditary HUS is of course caused by gene mutations including coagulation pathways. Acquired HUS includes a more primary typical infection including Shiga toxin-producing E. coli (STEC), accounting for 90% of cases, and Streptococcus pneumoniae. Pneumococcal associated HUS typically affects infants and younger children and remains at less than 0.5%. These patients also present with pneumonia versus the common diarrheal episodes.
Causes
The causes of HUS is typically E. coli bacterial infection crossing into the intestines and thereby entering the bloodstream. Tiny blood vessels are damaged during this process “clogging” tiny vessels in the kidney, damaging the body’s filtering system and thereby causing acute kidney failure. Typically, the culprit is undercooked or spoiled food. Another commonality is thawing meats, dripping onto other food contaminated in the refrigerator or during the processing of preparing meat. Exposure to contaminated water can also be a factor.
Diagnosis
HUS is commonly diagnosed by the standard triad below:
- Hemolytic anemia- diagnosed by hemoglobin of less than 8 g/dl.
- Thrombocytopenia- characterized by a platelet count of less than 140,000.
- Acute kidney injury-diagnosed by elevated serum creatinine along with elevated BUN levels and low urine output. Hematuria and proteinuria may also occur.
Management
HUS is managed with supportive treatment, including fluid volume replacement therapies with IV fluids and IV nutritional supplementation. Adequate nutrition, reduction of nephrotoxic drugs, appropriated therapy, and of course fluid and electrolyte management. Blood transfusions and/or platelet transfusions are also warranted. The body is volume depleted and blood transfusions help the body fight this infection. Approximately 50% of cases require dialysis. Typically in the pediatric intensive care units continuous renal replacement therapy is performed by a pediatric intensivist along with a pediatric nephrologist. If the kidney function does not fully recover this is required at home as well. Children that do fully recover require ongoing follow-up and management by a pediatric nephrologist. The damage to the kidneys is so acute and harmful, they can later develop proteinuria or hypertension issues, resulting in chronic kidney disease at an early age.
Conclusion
HUS is a very complex disorder and can be extremely disruptive to a child’s psychological health as well. These children typically stay several weeks in the pediatric intensive care unit and are managed by a multidisciplinary team. Unfortunately, not every child survives this complex disease, however today since there are more medical resources and developments nearly 85% of children survive this disorder. Prompt evaluation and experience of the medical field is necessary to ensure survival.
References:
Gülhan, B., & Özaltın, F. (2021, September). Hemolytic uremic syndrome in children. Turkish archives of pediatrics. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8848578/
The Children’s Hospital of Philadelphia. (2014b, August 24). Hemolytic uremic syndrome in children. Children’s Hospital of Philadelphia. https://www.chop.edu/conditions-diseases/hemolytic-uremic-syndrome-children
Hemolytic uremic syndrome (HUS). National Kidney Foundation. (2022, January 3). https://www.kidney.org/atoz/content/hemolytic
Overview of hemolytic uremic syndrome in children. UpToDate. (n.d.-b). https://www.uptodate.com/contents/overview-of-hemolytic-uremic-syndrome-in-children?search=hus&source=search_result&selectedTitle=1~150&usage_type=default&display_rank=1
Invasive infections associated with GAS have been reported with increasing frequency, predominantly from North America and Europe.
Invasive infections associated with GAS have been reported with increasing frequency, predominantly from North America and Europe.
